Dr. Dilip Kumar Kowkonda
Hyderabad Smiles is considered the best dental clinic in Madhapur, Hyderabad, India. With advanced technology and the latest equipment. Hyderabad Smiles offers a wide range of dentistry specialties under one roof, backed by cutting-edge technology and a world-class dental laboratory.
Why Choose Us
At Hyderabad Smiles, our clients experience personalized dental care
We have responsibly re-imagined dental care to seamlessly incorporate heartwarming hospitality with innovative health care facilities, world class technology, & quintessential services. Our pioneer setup boasts dental treatments devoid of any fear or anxiety.
Meet Our Team
Dr. Dilip Kumar
Dr. Naaga Deepika
Dr. Shireesha
Dr. Abhishek
Dr. K.Sandeep
Dr. Nirali Shah
Dr. Mayuri
Dr. Saipallavi
Dr. Devika Chakravarty
FAQ' s
People do not regularly visit a dentist. They take appointment only when they have a problem. While people feel they are saving money, it often ends up costing much more in cost and time. Many dental problems do not have symptoms until they reach the advanced stages. It always better to visit best dental hospital in Hyderabad, for regular check-ups and prevent any oral issues before they turn into serious problems.
Hyderabad Smiles is the best dental clinic in Hyderabad, you can get the best treatment and at affordable costs.
There are many dental hospitals in Hyderabad where you can get the treatment for your dental problems. Hyderabad Smiles is the one stop destination for all your dental problems. It has three branches across the city to reach people and serve them better
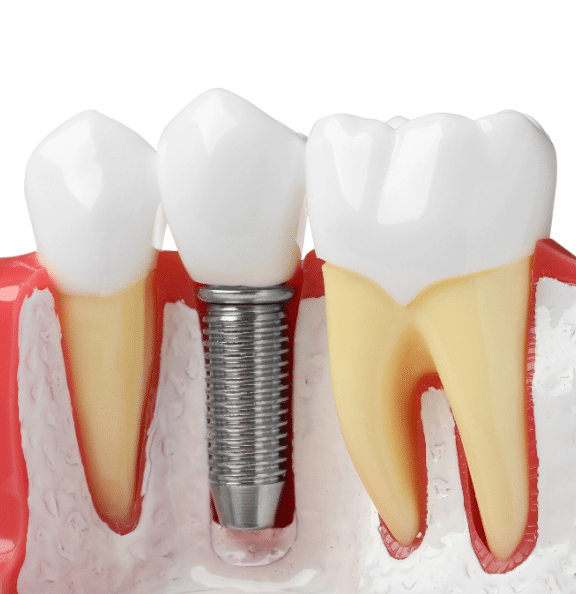
Dental implants are considered to be one of the costliest treatment and time taking. At Hyderabad Smiles, the treatment is done at affordable cost and in quick time based on the health condition of the patients
Dental care is really important for any person, if a person have oral health issue then it will take some time to recover completely and also based on the type of problem the cost will also be charged.